What is thumb arthritis?
Thumb arthritis is osteoarthritis of the thumb base. Responsible for painful discomfort in hand use, it affects women more often than men.
The trapezium is a small, roughly cubic bone of 1.5 to 2cm per side, at the thumb base, which receives throughout life, with each thumb movement, 10 times the pressure exerted by it. It is therefore a joint frequently affected by osteoarthritis, like the knee or hip.
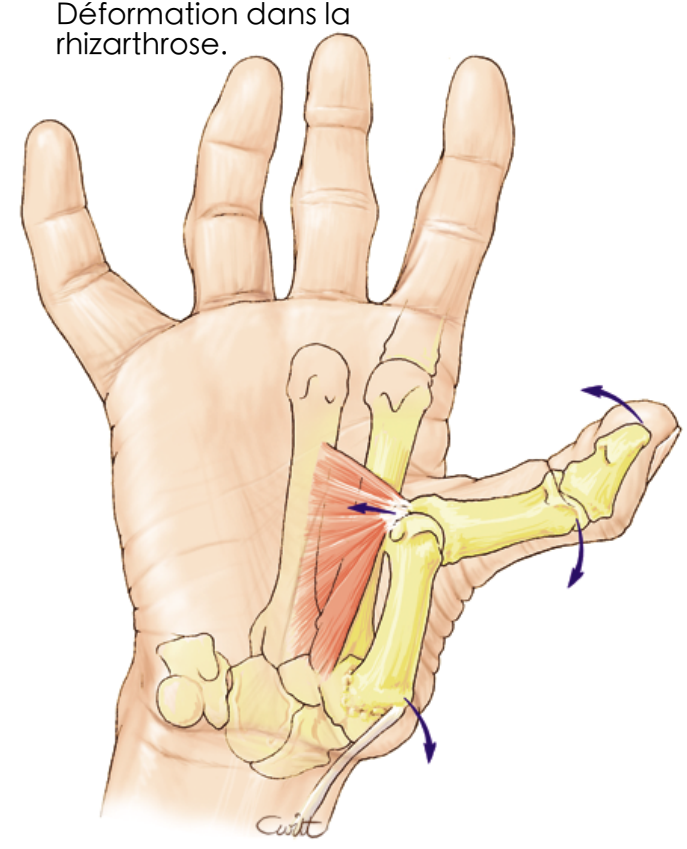
Deformation in thumb arthritis
How does thumb arthritis usually present?
The 3 main signs are pain, deformations and loss of strength.
Pain
Pain is located at the thumb base, near the wrist, on the anterior and dorsal surfaces. Direct palpation, movements and forceful gripping of objects between thumb and index finger awaken these pains, sometimes associated with cracking.
Deformation
Thumb deformation occurs in advanced cases. As a consequence of joint destruction and progressive ligament distension, the metacarpal "slides" toward the dorsal surface and initiates deformation, maintained and accentuated by successive muscle retractions. This produces the classic M-shaped thumb.
Loss of strength
Pain and deformation reduce the possibilities of thumb use and therefore of the hand, which progressively loses strength through muscle deconditioning.
A simple X-ray allows diagnosis of the disease and its evolutionary stage.
I have thumb arthritis, what can be done?
There is no immediate relationship between the extent of radiographic joint destruction and symptom intensity. Some minimally destroyed joints cause significant pain, and conversely, major radiographic osteoarthritis is relatively well tolerated.
It is therefore not necessary to be alarmed, and treatment may not be necessary... for the moment.
Splint treatment
When pain and discomfort increase, splint treatment is initially proposed. Joint rest in splints at night and occasionally during the day allows the hand to be freed for less painful use periods.
Infiltrations
Possibly, a corticosteroid infiltration or viscosupplementation with hyaluronic acid can reduce an osteoarthritic flare or allow waiting a few months, but they will not change the medium and long-term evolution.
Surgery
If splint treatment is ineffective, or if managing their use is not suitable, an operation can be performed. Your doctor and surgeon are your best advisors to assist you in these choices.
I'm going to have thumb arthritis surgery... what will happen to me?
Surgical treatment of thumb arthritis has been practiced for a long time and depends on the disease stage, hand use, age, and extent of cartilage and bone destruction.
Arthroscopy (moderate damage)
When damage is moderate, arthroscopic joint "cleaning" can be proposed, possibly combined with "lubricant" injection. It is a waiting treatment before more substantial surgery, but rarely practiced as results are unpredictable.
Trapezectomy (classical treatment)
The most classical treatment consists of removing the worn trapezium bone (trapezectomy), responsible for pain, and replacing it with a "cushioning pad". The surgeon then uses a tendon rolled on itself or fashions a tendon hammock for the thumb base, or uses cartilage from a rib when the patient is very young or physical and professional activity requires much strength.
The result requires several months to stabilize, but strength and endurance are variable.
Trapeziometacarpal prosthesis "Maïa"
When damage is less severe and thumb use is more normal, particularly in a woman over 50 years old, a so-called trapeziometacarpal metal prosthesis can be implanted.
Recovery is much faster and more predictable, but at the cost of the disadvantage of implant replacement when worn, around 10 to 15 years after initial surgery.
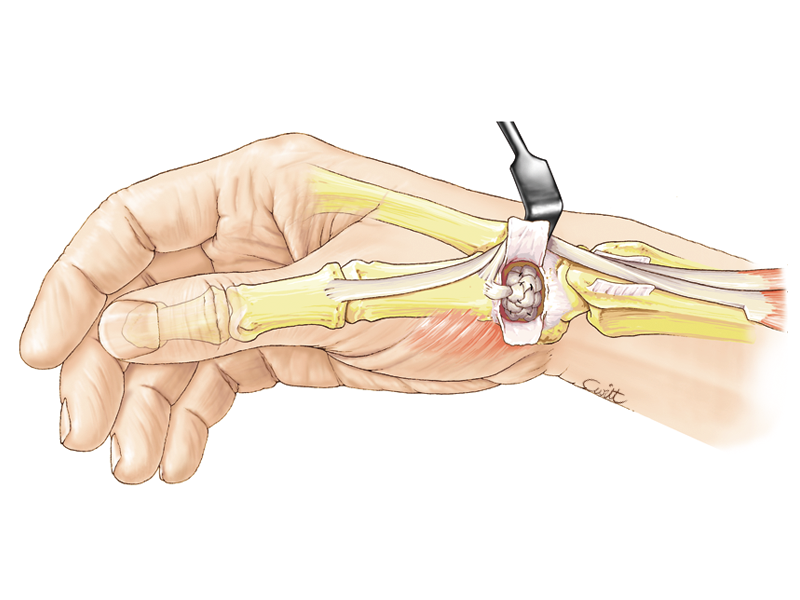
Trapezectomy and creation of a "tendon cushion"

Metal prosthesis "Maïa"
Hospitalization and recovery - Trapezectomy
Hospitalization is 2 days, the procedure performed under regional anesthesia. A pin or splint is left in place for 4 weeks to protect repairs, before physiotherapy starts.
Hand convalescence takes around 3 to 6 months.
Hospitalization and recovery - Prosthesis
For a prosthesis, a splint is worn for protection for 2 weeks, then physiotherapy or self-rehabilitation starts. Strength activities are started from 2 months.
Effectiveness on pain is often very satisfactory, improving hand function.
Is thumb arthritis surgery risk-free?
No, of course not. Although it is a codified, routine and mastered procedure, the risk exists, as with any surgery, even if complications are rare.
We mainly find, even if all precautions are taken:
- Healing difficulties
- Hematoma
- Local infection
- Algodystrophy
- Anesthetic complications
- Section of a very fine branch of the radial nerve
- Scar hypersensitivity
- Early wear or dislocation of a prosthesis
- Allergy to prosthesis material
What is the risk of not having surgery?
Being a functional surgery, there is no risk in not having the operation.
As osteoarthritis continues its work, pain, deformations and discomfort increase, as much as hand comfort and function deteriorate.
Do you suffer from thumb arthritis?
Our specialists offer you personalized care to relieve your pain and restore optimal thumb function.
Make an appointment